Screwless Dental Implants: A Presentation of Modern Solutions in the United States
“Screwless” implant dentistry is a common term, but it can mean different things in clinical practice—from crowns that are cemented instead of screw-retained to implant systems designed to lock components together without an abutment screw. For U.S. patients considering implant treatment, understanding what is truly screwless (and what is not) can make it easier to evaluate comfort, stability, maintenance needs, and long-term outcomes.
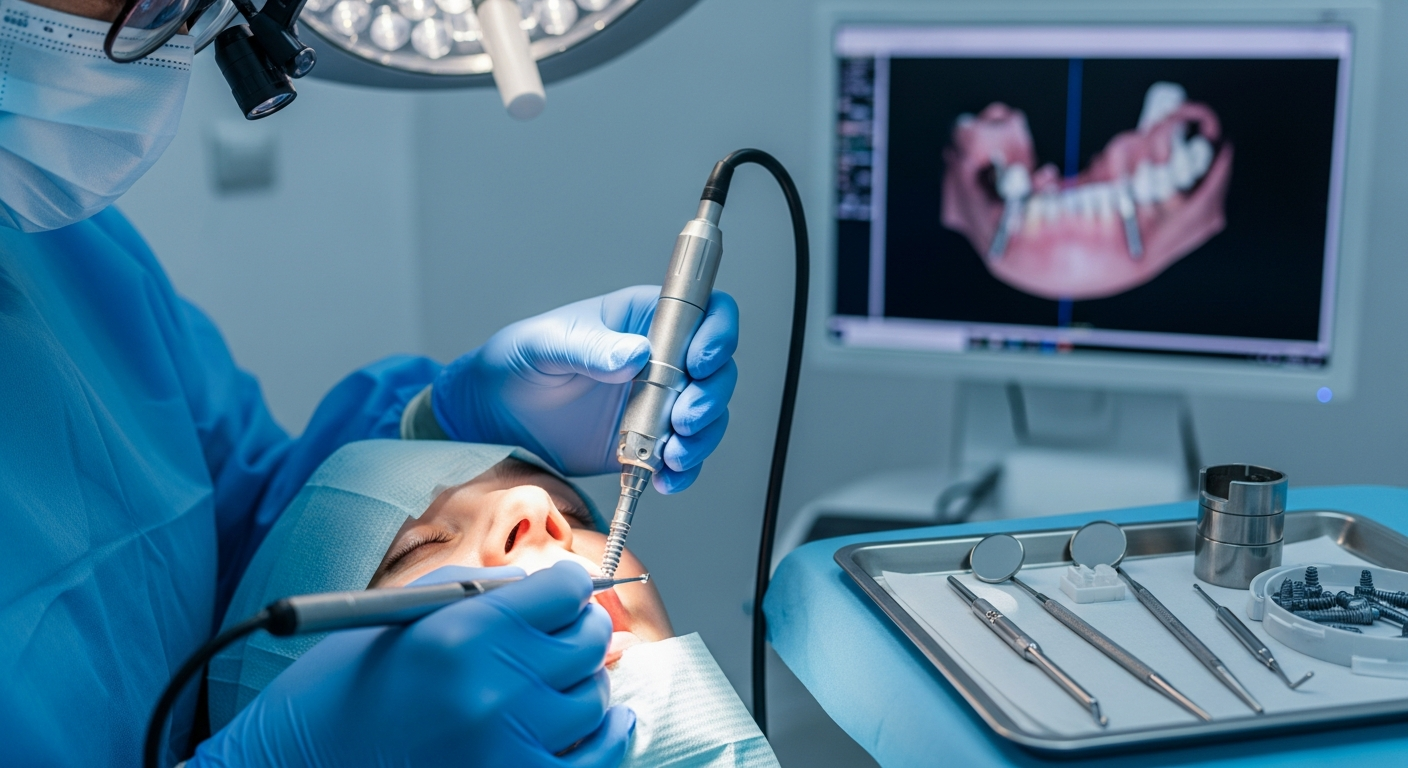
Choosing an implant solution often involves more than picking a brand or a single technique. The way a crown is attached to an implant, how components connect, and how the bite forces are managed can influence day-to-day comfort and long-term maintenance. In the United States, “screwless” approaches are typically discussed as alternatives to screw-retained restorations, but the term is not always used consistently.
Public understanding of alternative dental implant technologies
In everyday conversations, “screwless” may be understood as an implant that does not use any screw at all. Clinically, it more often refers to the way the visible tooth (the crown) is retained: either by a small access hole for a crown screw (screw-retained) or by cement bonding the crown to an abutment (cement-retained). Some implant systems also use locking-taper or conical connections designed to reduce micro-movement and can be described as screwless at the abutment level.
Alternative dental implant technologies can also include different materials and workflows, such as titanium versus zirconia implants, conventional impressions versus digital scans, and stock components versus custom-milled abutments. These choices are not inherently “better” or “worse,” but they can change how repairs are handled, how the gumline looks, and how easily the restoration can be retrieved for maintenance.
Factors influencing comfort, stability and long-term integration
Comfort and stability depend heavily on biology and bite mechanics, not just on whether a crown has a screw. Bone quality and quantity, gum health, and the patient’s bite forces (including clenching or grinding) influence how an implant integrates and how the restoration performs over time. Surgical placement angle and depth also matter because they affect how forces transfer into the jaw and how the final crown emerges through the gum.
Long-term integration is supported by consistent oral hygiene and professional maintenance. Inflammation around implants (often discussed as peri-implant mucositis or peri-implantitis) can compromise stability regardless of restoration type. For some patients, a screw-retained crown can make periodic removal and cleaning simpler, while cement-retained designs can require extra care to avoid residual cement at the gumline.
Key differences between traditional and screwless implant systems
Traditional screw-retained restorations typically include a crown that is attached to the implant (or to an abutment) with a small screw, leaving a circular access opening that is later filled. One practical advantage is retrievability: if a crown chips, if a component loosens, or if the implant needs inspection, the dentist can often remove the crown without cutting it off.
Screwless approaches most commonly mean cement-retained crowns, where the crown is bonded onto an abutment. This can improve the appearance of the chewing surface because there is no screw-access filling. However, cemented crowns may be harder to retrieve and, if cement is left under the gum, it can increase the risk of irritation. Separately, systems marketed as screwless at the implant–abutment interface may use a locking-taper or friction-fit connection; these designs aim to reduce screw-related complications, but they still require precise technique and case selection.
Modern approaches to screwless dental implants in the United States
In U.S. clinical settings, modern “screwless” planning often focuses on matching the retention method to the patient’s anatomy and risk profile rather than applying one method to every case. Digital treatment planning and guided surgery can help position implants more accurately, which is relevant because implant angle influences whether a screw-retained crown would place an access hole in a visible area. When esthetics are a priority, clinicians may plan for cement-retained restorations or for angled screw-channel solutions that keep screw access off the front surface.
Another modern approach is using patient-specific components, such as custom abutments or custom hybrid restorations, to better manage gum contours and emergence profile. These workflows can be paired with either screw-retained or cement-retained designs. For patients with heavy bite forces or a history of restoration fractures, the restorative material choice (for example, monolithic zirconia versus layered ceramics) and occlusal design can be as important as the presence or absence of a screw.
Practical considerations when evaluating implant solutions
When evaluating implant solutions, it helps to ask the dentist to clarify what “screwless” means in the proposed plan: a cemented crown, a friction-fit connection, or another approach. Practical questions include how the restoration will be maintained, what happens if it needs repair, and how the team will reduce known risks such as excess cement, loosening, or chipping. It is also reasonable to discuss how the plan addresses gum health and cleaning access, especially for patients with a history of periodontal disease.
A balanced decision typically considers clinical factors (bone volume, smile line, bite forces), maintenance factors (retrievability and cleaning), and personal preferences (appearance and comfort). Because implant treatment is individualized, two patients in the same city may receive different solutions that are both appropriate. This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Implant dentistry in the United States continues to evolve toward more precise planning, more customized components, and clearer alignment between a patient’s risk factors and the restoration design. Understanding the real meaning of “screwless,” along with the tradeoffs in maintenance and retrievability, can help patients have more informed conversations about comfort, stability, and long-term integration.






